Understanding Prostate Cancer: The UK's Biggest Male Cancer
Prostate cancer begins in the prostate gland, a small organ located just below the bladder that contributes to seminal fluid. This disease represents the most significant cause of cancer in men across the United Kingdom, with approximately 55,300 new diagnoses and 12,200 deaths annually. While it's the second most common cancer overall after breast cancer, its impact on the male population is substantial. The nature of prostate cancer varies significantly between individuals; for many men, it grows slowly, while in others it can develop and spread more aggressively.
Recognising Symptoms and Understanding Risk Factors
During its early stages, prostate cancer typically presents no obvious symptoms, which contributes to many late diagnoses. However, certain changes should prompt a conversation with your GP. "People should speak to their doctor if they notice changes to how often or easily they pee, spot blood in their pee, or have difficulty getting or keeping an erection," advises Naser Turabi, Cancer Research UK's director of evidence. He emphasises that while these symptoms often indicate other health conditions or natural ageing, early detection of cancer can be life-saving.
The signs of advanced prostate cancer differ markedly and include unexplained weight loss, persistent tiredness, and back or bone pain that doesn't resolve. While age increases risk for all men, certain groups face significantly higher probabilities of developing the disease. Black men are approximately twice as likely as white men to both develop and die from prostate cancer. Family history also plays a crucial role; having close relatives with prostate, breast, or ovarian cancer increases risk, particularly if they carried the BRCA1 or BRCA2 gene variants.
Diagnosis, Testing and Treatment Options on the NHS
The diagnostic process for prostate cancer involves multiple steps rather than a single definitive test. Any man or transwoman over 50 can request a prostate specific antigen (PSA) blood test from their GP through the NHS. Professor Kamila Hawthorne, chair of the Royal College of GPs, explains that the initial consultation involves taking a careful medical and family history, discussing why the patient is requesting the test, and outlining the risks and benefits of PSA testing.
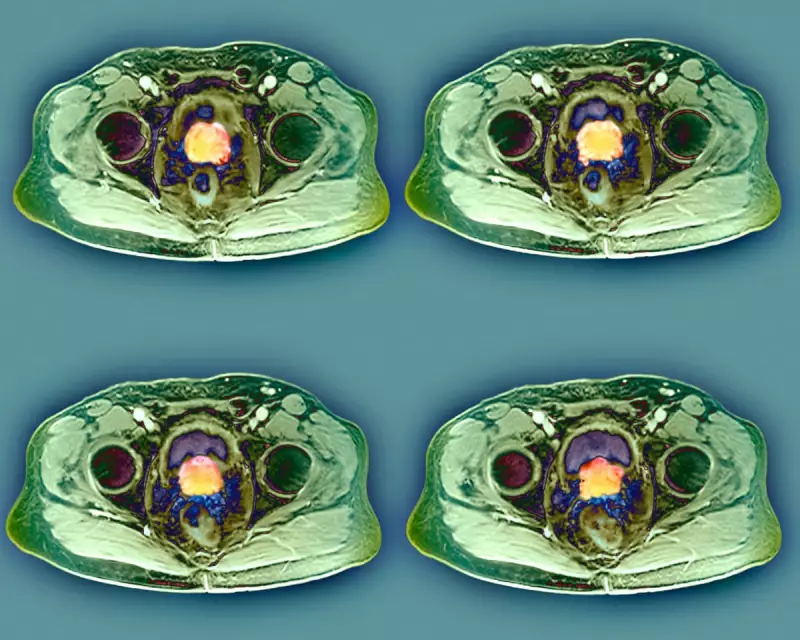
However, PSA tests have limitations, including potential false positives and false negatives. When results show elevated PSA levels, patients are typically referred for an MRI scan and, if necessary, a biopsy for definitive diagnosis. Modern biopsy techniques have become significantly less invasive, with transperineal biopsies (through the skin between the scrotum and anus) now preferred over rectal approaches due to lower infection risks.
Treatment approaches vary depending on how early the cancer is detected and its likely growth rate. Options include surgery, radiotherapy, and hormone treatment. For many men with early-stage, slow-growing prostate cancer, immediate treatment isn't always necessary. Instead, they may be offered 'active surveillance' involving regular PSA tests, check-ups, and occasional scans or biopsies, with treatment beginning only if the cancer shows signs of progression.
The Critical Importance of Early Detection
Despite available testing, too few men seek PSA tests, particularly those from poorer backgrounds, less educated demographics, and minority ethnic groups. Dr Jayne Spink of Prostate Cancer Research notes this means "we are still diagnosing far too many men when their cancer is already advanced and becomes incurable."
The survival statistics underscore why early detection matters tremendously. Survival rates have more than tripled since the 1970s, with more than 80% of men diagnosed now surviving their disease for 10 years or more, compared to just 22% fifty years ago. When caught at stages 1 or 2, over 85% of men live at least 10 years post-diagnosis. However, once the cancer reaches stage 4 and spreads widely, long-term survival drops sharply to approximately 19%.
To reduce prostate cancer risk, Cancer Research UK recommends proven steps including stopping smoking, maintaining a healthy weight, and eating a balanced diet. For those with specific risk factors, such as black men over 45 or individuals with strong family histories of relevant cancers, proactive discussions with GPs about regular PSA testing are strongly advised.









