Kenya's HIV Prevention Jab Rollout Leaves Hardest-Hit Communities Behind
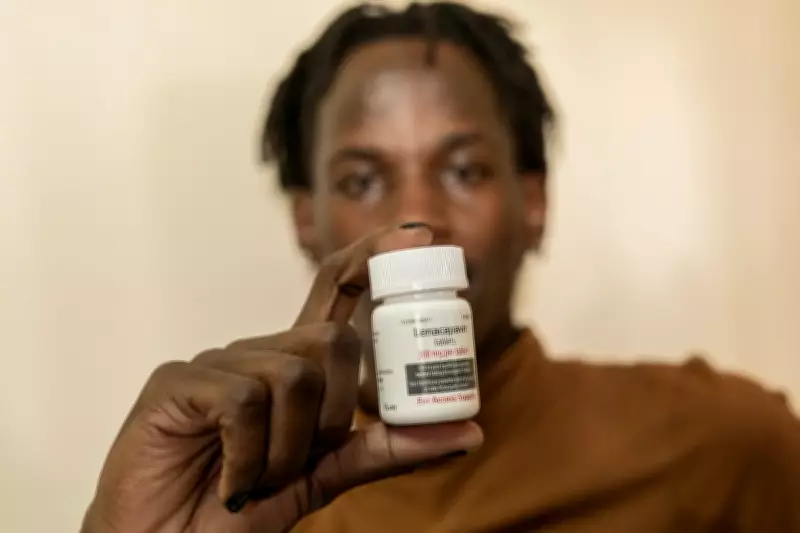
Kenya has embarked on a pioneering initiative to distribute lenacapavir, a groundbreaking HIV prevention injection hailed by scientists as the closest development yet to a vaccine for the virus. This rollout aims to mark a decisive step in the global fight against HIV, targeting the 1.4 million Kenyans living with the virus and many more at risk. However, a charity has raised alarms that the program is not reaching those who need it most, particularly in high-prevalence informal settlements.
Exclusion of High-Risk Areas
Last month, Kenya became one of the first countries globally to begin distributing lenacapavir, intended to substantially reduce new HIV infections by 2030. Yet, in the dense sprawl of Kibera—one of Africa's largest informal settlements—this future feels distant. Kibera has been omitted from the priority areas selected for the initial phase of the rollout, despite HIV prevalence in Nairobi's informal settlements estimated at around 12 percent, more than double the roughly five percent recorded in non-slum urban areas.
The initial rollout will see 21,000 doses distributed across 152 health facilities in 15 high-burden counties. Notably, the Tabitha Medical Clinic—the main health facility operated by CFK Africa, a long-standing community organisation in Kibera—is not among them. Jeffrey Okoro, the organisation's chief executive who grew up in Kibera, expresses frustration over the exclusion.
"I've seen firsthand how devastating HIV and AIDS can be. As an organisation, we welcome the national rollout. But in communities like Kibera, lenacapavir could be a game-changer. Right now, it's not reaching the people who would benefit most," Okoro tells The Independent. He adds that they have received no explanation for the omission or indication of when it might change.
Barriers to Access
In theory, residents of excluded areas can travel to designated facilities elsewhere in Nairobi. In practice, this presents significant barriers. The nearest approved sites are between roughly 1.5 and 3.5 miles away, with a one-way journey costing between 220 and 380 Kenyan shillings—equivalent to £1.30 to £2.20. For residents living on less than £1.50 a day, this often forces a choice between transport and food.
"People prefer to go to clinics they know and trust," Okoro says. "If you push everything into national hospitals, you exclude the very people you say you are targeting." These structural challenges are not new; past efforts to improve retention on HIV treatment in Kibera have shown how persistent barriers like transport costs and travel time can be, with recent trials offering incentives finding no meaningful improvement in patient adherence.
Cost and Equity Concerns
Currently, the drug is being offered free during the initial rollout, but concerns loom about future costs. Officials indicate that if scaled up, lenacapavir could cost around 7,800 Kenyan shillings per year—heavily subsidised but still a significant outlay in low-income communities. Agreements involving the Clinton Health Access Initiative and the Gates Foundation aim to reduce the price to around £30 per patient annually across over 120 low and middle-income countries, but this depends on generic versions expected from 2027, with supply remaining limited until then.
This situation raises broader concerns that scientific breakthroughs are outpacing the systems needed for equitable delivery. Antonio Flores, a senior HIV adviser at Médecins Sans Frontières, warns: "Without deliberate policy choices, access will remain uneven." Kenya's health authorities insist this stage is only the beginning, but access, rather than efficacy, may prove the decisive factor in the rollout's success.
Community-Based Solutions
Okoro advocates for a community-rooted approach to bridge the gap. He argues that using existing networks of health promoters, youth centres, and local organisations could deliver the drug and ensure patients return for their second injection six months later. Lenacapavir's dosing schedule makes such a model feasible.
"You could attach someone to a youth centre, follow up with them, remind them when their next injection is due. That's how you build something that actually works," he says. This approach contrasts with current efforts that fail to meet people where they are, as Okoro notes: "The issue isn't motivation, people want to stay healthy. But the system doesn't meet them where they are."
Glimpses of Hope and Ongoing Challenges
At included sites like Riruta Health Centre, patients express relief and optimism. Teresia Wanjiku describes the injection as long overdue: "I have been waiting for this for many years. It is much easier than taking pills every day." For those who can access it, lenacapavir represents a profound shift towards a future where HIV is no longer a constant threat.
However, in places like Kibera, it remains—for the moment—a breakthrough just out of reach. The rollout highlights a critical need for policy adjustments to ensure that transformative health innovations benefit all, especially the hardest-hit communities. As Kenya moves forward, the success of this initiative will depend on addressing these disparities and fostering inclusive access to life-saving prevention tools.









