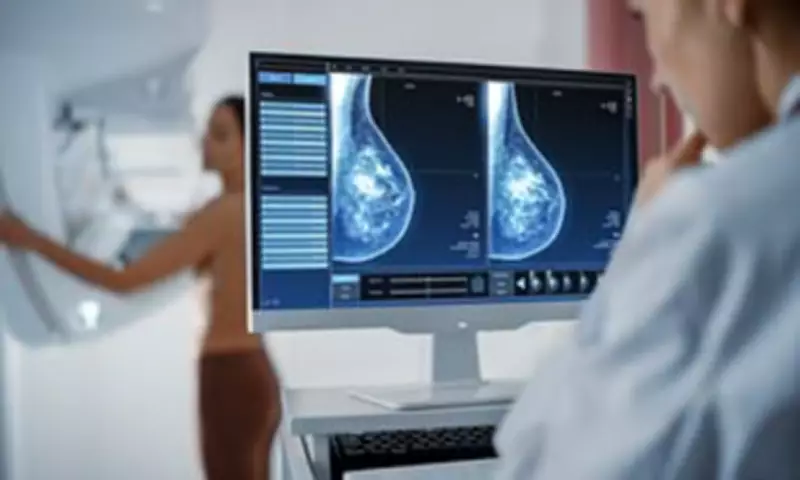
Cancer Patients Face Diagnosis Delays Under Labour's NHS Reforms, Doctors Warn
Cancer patients could experience significant delays in diagnosis and treatment under Labour government plans to reduce what it terms 'unnecessary' medical appointments, according to warnings from senior doctors and medical organisations. The controversial policy centres on an expanded 'advice and guidance' (A&G) process that requires general practitioners to consult specialists before making hospital referrals in cases where such consultation is deemed clinically appropriate.
How the Advice and Guidance System Works
The A&G system involves GPs seeking specialist medical opinions through telephone consultations, email exchanges, or other digital communication methods rather than immediately referring patients to hospital outpatient departments. NHS England describes this approach as a 'key part' of its strategy to avoid unnecessary hospital appointments, with ministers claiming it enables patients to begin more appropriate treatment sooner and prevents thousands from waiting weeks for potentially pointless consultations.
However, medical professionals have raised serious concerns about the implementation of this system. GPs report instances where specialists have downgraded urgent cancer referrals to A&G requests instead of accepting them as direct referrals, creating what doctors describe as a significant risk of missed or delayed cancer diagnoses.
Rising Demand and Specialist Workload Concerns
The Royal College of Physicians (RCP) has issued a stark warning about the growing pressure on the A&G system. According to NHS England figures released last week, the total number of A&G requests reached 305,000 in February alone - representing a substantial 26 percent increase compared to the same period last year.
Across all types of specialist medical advice, total requests have soared to approximately 1.1 million, nearly doubling since records began in April 2022. The RCP anticipates further growth in demand as A&G becomes embedded within the standard GP contract, potentially overwhelming specialist doctors who must maintain their direct clinical services while managing escalating volumes of advisory work.
Medical Leaders Voice Patient Safety Concerns
Professor Mumtaz Patel, president of the Royal College of Physicians, expressed grave concerns about the potential consequences for patient care. 'Our concern is that if patients face delays in accessing specialist input, conditions may worsen before the right care is provided,' she stated. 'When that happens, people can end up seeking help in emergency care because they feel they have nowhere else to turn.'
Professor Patel emphasised that healthcare reforms must not create new barriers to timely specialist care or inadvertently push more patients into an already overstretched urgent and emergency care system.
Dr Katie Bramall, chairman of the British Medical Association's GP committee, has previously described the risks associated with A&G as 'a huge concern for every single GP I meet and speak to.' She added that 'it should be a huge concern for every patient too,' characterising the policy as 'awful for patients' and politically motivated rather than clinically driven.
Specific Cases Highlight Potential Dangers
The Wessex Local Medical Committee, representing GPs in that region, provided a concrete example of the system's potential failings. 'When a GP assesses that a patient needs specialist care, that assessment can now be overridden remotely - by a clinician who has not seen the patient,' the committee stated.
They described a specific case in their region where an urgent cancer referral was converted to an A&G response multiple times rather than being accepted as a direct referral, potentially delaying the eventual diagnosis. Such incidents have heightened concerns among medical professionals about patient safety under the new system.
Political Controversy and Government Response
The Conservative opposition has criticised the A&G process as essentially a form of healthcare rationing, accusing the Labour government of manipulating statistics to artificially suppress hospital waiting list numbers. This political dimension adds further complexity to an already contentious healthcare policy debate.
A Department of Health and Social Care spokesperson defended the initiative, stating: 'The advice and guidance initiative is giving patients faster access to specialist expertise without needing to wait for a hospital appointment, helping to get people the right care faster and reduce unnecessary referrals which waste vital clinical time.'
The spokesperson also referenced the forthcoming 10 Year Workforce Plan, which promises to outline strategies to support doctors and improve their working conditions, aiming to ensure the NHS has appropriate staffing to meet future healthcare demands.
As the debate continues, medical professionals remain concerned that well-intentioned efficiency measures might inadvertently compromise patient care, particularly for those with serious conditions like cancer where timely diagnosis and treatment can be matters of life and death.