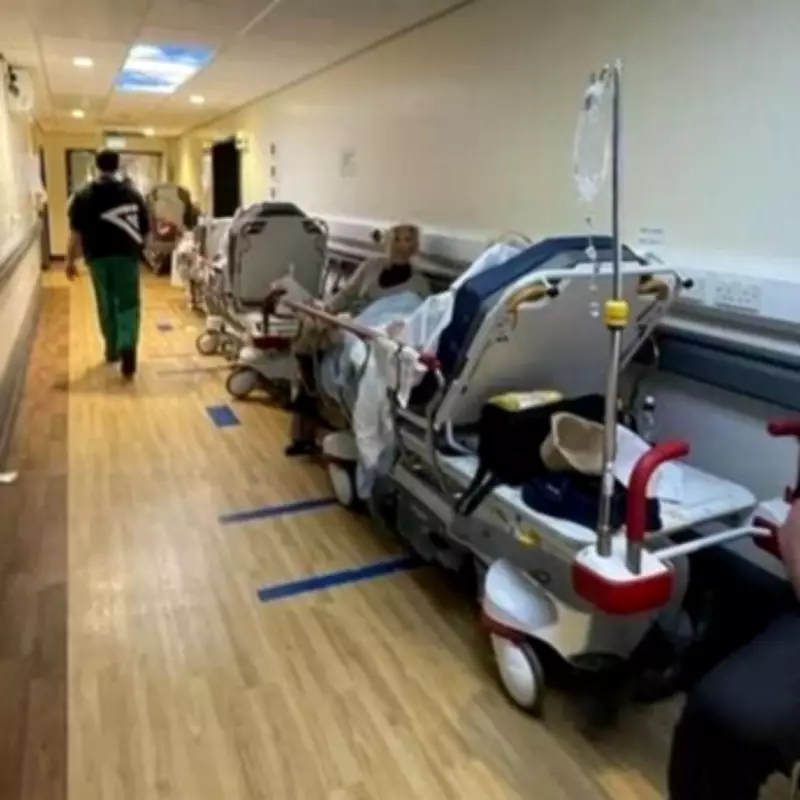
Nurses and doctors across the National Health Service are reportedly too ashamed to look patients in the eye, a direct consequence of the escalating hospital corridor care crisis. This alarming revelation was presented to MPs during a recent Health and Social Care Committee session, where staff leaders branded the situation a "national scandal" that is actively contributing to thousands of patient deaths each year.
A National Scandal Unfolding in Corridors
Corridor care, where patients receive treatment in hallways, store cupboards, and other unsuitable spaces, has transitioned from a temporary makeshift solution to a permanent and dangerous reality in many NHS hospitals. Patients are frequently left waiting for hours on trolleys before admission to proper wards, creating unsafe conditions that medical professionals argue are fundamentally unacceptable.
Expert Warnings and Statistical Evidence
Dr Ian Higginson, President of the Royal College of Emergency Medicine (RCEM), delivered a stark warning to the committee. "Corridor care is a visible symptom of overcrowding, which is a national crisis and, I believe, a national scandal," he stated. "There is absolutely no safe or acceptable way to provide care for patients in corridors… it just cannot be done. We cannot understand why this hasn't got the focus it deserves because it's actively killing patients."
Supporting this claim, NHS data reveals a chilling correlation: patients who spend over twelve hours in Accident and Emergency departments are more than twice as likely to die within thirty days compared to those seen within two hours. A survey published by the RCEM found that more than half of Emergency Department Clinical Leads in England consider their A&E units unsafe for patients.
The Human Cost and Staff Morale
Dr Higginson provided a conservative estimate that approximately 16,000 patients die annually due to long waits in emergency departments. "If this was any other sector there would be howls of rage. If it was an airline, we would be grounding aircraft," he remarked, highlighting the severity of the issue.
The crisis is taking a profound psychological toll on healthcare staff. Professor Nicola Ranger, General Secretary of the Royal College of Nursing (RCN), explained that nurses feel deep shame when unable to provide dignified care. "Nurses are often the ones closest to the patient. For many of them, that's what they feel very ashamed about as well, when they know that someone is stuck on a nurse's station and they need the toilet, or they're dying and they need a quiet space," she said.
Professor Ranger added, "I was talking to a patient there last week who said, it's that [nurses] feel embarrassed. So there's a lack of eye contact now. That is a symptom of people just, you know, head down because they feel upset with what they're seeing." Dr Higginson confirmed experiencing this phenomenon personally, noting that staff often struggle to face patients in overcrowded waiting rooms.
Historical Context and Escalating Numbers
The problem of extended A&E waits has worsened significantly over the past decade. Before the Conservative government's tenure, twelve-hour waits were virtually unheard of. By December 2019, 2,356 patients waited over twelve hours on trolleys for a bed. Shockingly, by December 2025, this number had skyrocketed to 50,775 patients.
Elderly patients are disproportionately affected, enduring the longest waits. A 2024 RCN report documented instances of patients dying "under a pile of coats" in packed waiting rooms, underscoring the dire circumstances.
Investigative Findings and Systemic Failures
Dr Rosie Bennyworth, Chief Executive of the Health Services Safety Investigation Board, informed MPs that investigations uncovered patients being treated in corridors, store cupboards, kitchens, and various other areas never designed for clinical care. This ad-hoc approach compromises both patient safety and staff ability to deliver effective treatment.
Proposed Solutions and NHS Reforms
In response to the crisis, the NHS announced operational changes last month aimed at alleviating pressure on emergency departments. A new blueprint outlines the creation of dedicated areas for patients requiring "extended" care, specifically targeting those likely to stay in A&E for four to eight hours. These Extended Emergency Medicine Ambulatory Care Areas (EEMACs) are intended to make prolonged waits more bearable, particularly for elderly patients whose risk of death increases significantly with delays.
The strategy also emphasises improved triage upon arrival, redirecting suitable patients to same-day clinics for faster, more appropriate treatment. Labour and NHS England have set an interim target for March 2026, aiming for 78% of A&E patients to be admitted, discharged, or transferred within four hours. Current data shows 73.8% of patients in England are seen within this timeframe.
Despite these measures, medical professionals remain deeply concerned. The corridor care crisis represents not only a logistical failure but a profound ethical challenge, eroding the foundational trust between healthcare providers and the public they serve. As staff grapple with embarrassment and patients face increased mortality risks, urgent and sustained action is demanded to restore safety and dignity to emergency healthcare in the UK.









