Eswatini's Struggle Against HIV: A New Drug Brings Hope and Challenges
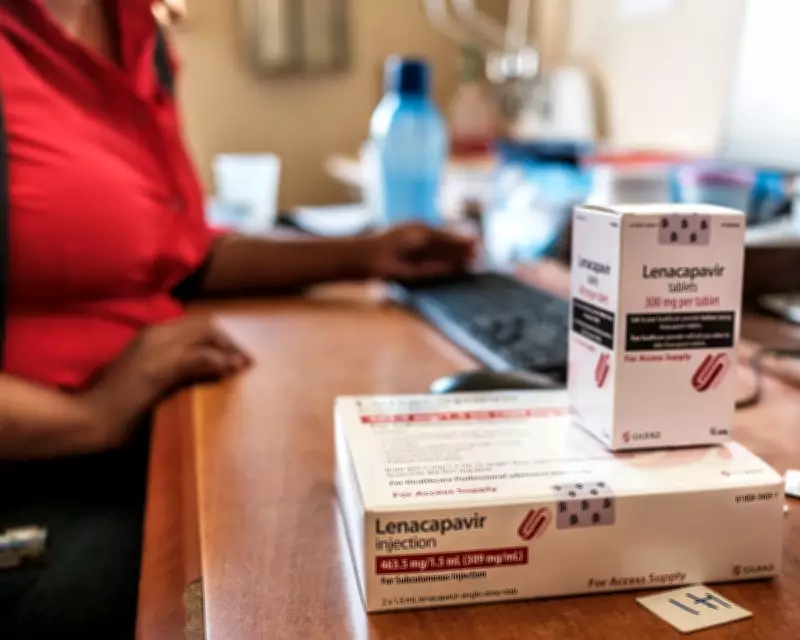
In Eswatini, a small southern African nation formerly known as Swaziland, a groundbreaking drug called lenacapavir is offering a ray of hope in the fight against HIV. Administered as an injection every six months, this medication can prevent people from contracting the virus, earning it the nickname of a "miracle" drug among patients and clinicians. Eswatini is among the first countries globally to implement this innovative treatment, aiming to curb new infections in a region where HIV prevalence is alarmingly high.
The Dire Reality of HIV in Eswatini
Eswatini holds the unfortunate distinction of having the world's highest HIV prevalence, with approximately one in four people infected. Each year, the country records around 4,000 new HIV infections among its population of 1.2 million. The financial pressures on vulnerable groups, such as sex workers, exacerbate the crisis. For instance, Precious, a sex worker, faces a stark choice: charge 100 lilangeni (about £4.50) for protected sex or double that amount for unprotected encounters. This economic incentive highlights the risks in a nation where HIV is rampant.
During a recent clinic visit, Precious and five other sex workers underwent HIV testing, revealing that four were positive. Her personal story underscores the broader societal issues: after fleeing an abusive husband who broke her leg, she turned to sex work to support her two children and blind mother, reflecting the harsh realities for up to 60% of Eswatini's population living below the poverty line.
Lenacapavir: A Potential Gamechanger with Limited Reach
Lenacapavir, often referred to as "len," represents a significant advancement in HIV prevention. Unlike daily pills or other pre-exposure prophylaxis (Prep) methods like vaginal rings or shorter-acting injections, its six-monthly dosing offers convenience and improved adherence. Sindy Matse, programme manager for the Eswatini National Aids Programme, notes that previous methods faced challenges, such as forgetfulness with daily pills or discomfort with alternatives, making lenacapavir a highly anticipated solution.
However, the rollout is hampered by severe supply shortages. Dr Nkululeko Dube, country programme director for the Aids Healthcare Foundation Eswatini, describes the current doses as "not even a drop in the ocean" compared to the need. As of mid-March, only 2,995 people had started treatment, with clinics like Lobamba receiving just 130 doses and the central medical store holding a mere 730, many reserved for second doses. The Global Fund is providing 6,000 doses by 2026, but delays and US aid cuts have slowed distribution.
Funding and Access Barriers
The financial aspects of lenacapavir add another layer of complexity. In the United States, the drug costs $28,218 annually per patient, but through agreements with the Global Fund, poorer countries like Eswatini pay about $60 per person per year. Generic versions are expected to reduce this to $40 by 2027, potentially dropping to $25 with sufficient demand. Despite this, manufacturer Gilead has faced criticism for restricting access to cheaper supplies and refusing direct sales to humanitarian organisations, with Médecins Sans Frontières warning that such actions endanger vulnerable populations.
US funding cuts have further disrupted HIV prevention efforts across sub-Saharan Africa, leading to the closure of specialist services for high-risk groups, including men who have sex with men, transgender women, and drug users. In Eswatini, activists report difficulties in accessing care at mainstream clinics, where stigma persists, complicating the equitable distribution of lenacapavir.
Targeting High-Risk Populations
Eswatini's strategy prioritises key demographics for lenacapavir access, including teenage girls and young women, who account for three-quarters of new infections, as well as pregnant and breastfeeding mothers and sex workers. Matse emphasises that guidelines allow anyone requesting the drug to receive it, aiming to avoid stigmatisation. Yet, with an estimated 800,000 HIV-negative citizens, determining exact needs is challenging due to fluctuating risk levels and preferences.
For individuals like Princess, a 27-year-old sex worker supporting her children and siblings, access remains precarious. After being persuaded by an outreach worker to seek prevention, she faced a setback when a recent unprotected encounter required her to take post-exposure prophylaxis pills instead of lenacapavir, highlighting the ongoing barriers to consistent protection.
Future Prospects and Government Commitment
Despite current limitations, there is optimism about lenacapavir's long-term impact. Mark Edington of the Global Fund acknowledges that immediate effects on infection rates may be minimal this year but anticipates significant changes by 2027-28 with generic availability. Eswatini's health minister, Mduduzi Matsebula, views the drug as a gamechanger and is prepared to fund it domestically, aligning with the goal to end AIDS as a public health threat by 2030, or even 2028.
As Eswatini continues its battle against HIV, the success of lenacapavir hinges on overcoming supply shortages, securing sustainable funding, and ensuring inclusive access for all at-risk populations. The world watches closely, hoping this small nation can turn the tide against a devastating epidemic.









