Inside the 'Miracle' Drug Rollout That Could End Aids
A revolutionary new drug designed to prevent HIV infection, hailed as the closest equivalent to a vaccine, is currently being introduced in some of the world's most severely affected nations. Chief international correspondent Bel Trew reports from Eswatini in southern Africa, where there is renewed optimism that the pandemic might finally be brought to a close.
Death Sentence: The Real Cost of Aid Cuts on HIV
Lianne was merely 13 years old when she lost both her parents to Aids. Suddenly orphaned, she faced the daunting task of ensuring survival for herself and her younger sister. With insufficient funds to complete her education, no employment opportunities, and constant struggles to afford food, she felt compelled to turn to sex work as her only viable option.
Now aged 24, Lianne is acutely aware of the dangers in Eswatini, a southern African kingdom once labeled the epicentre of the HIV epidemic and still grappling with some of the highest infection rates globally. "Both my parents passed away. Hunger led me to join this work although I know it's risky," she explains, noting that she earns less than £25 weekly and cannot access HIV preventative medication, known as PrEP, independently.
However, hope has emerged in the form of Lenacapavir, dubbed the "miracle" drug, which the United Nations believes could safeguard millions like Lianne and potentially eradicate the Aids epidemic entirely.
The Groundbreaking Injection
This twice-yearly injection, described by the head of the UN Aids agency as "the closest thing we have to a vaccine," offers nearly complete protection against infection. Lenacapavir is being launched for the first time in nine of the most at-risk countries, including Eswatini, making Lianne among the initial recipients worldwide.
While this marks a significant advancement in HIV care, concerns persist regarding the rollout's scope and fears that its effectiveness may be limited without a global-scale implementation.
Impact of Aid Cuts
The positive developments surrounding Lenacapavir follow last year's devastating reductions in foreign aid spending by Donald Trump, which previously funded approximately half of Eswatini's HIV response. For Lianne, this meant the sudden closure of mobile clinics that provided free, life-saving HIV prevention therapy.
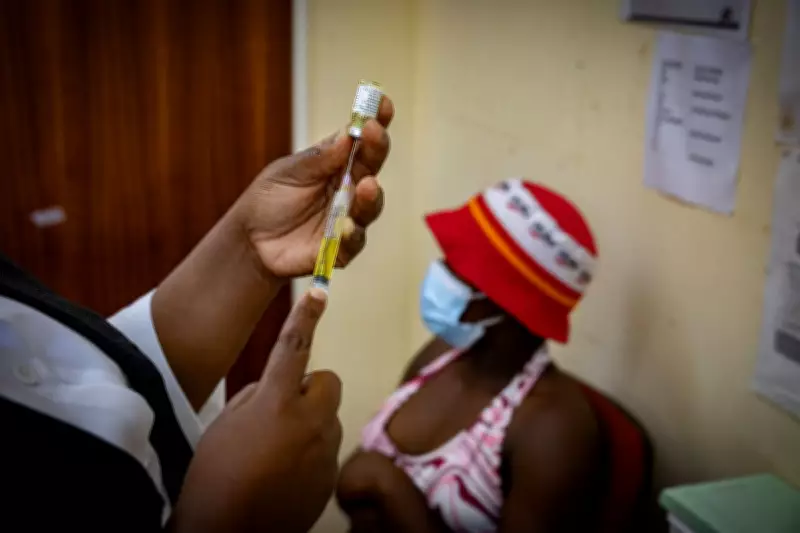
These closures have had deadly consequences: a friend and fellow sex worker recently died after contracting HIV and losing access to essential medication. "That is why I am so happy today, it's protection," Lianne expresses with relief as she receives the brightly coloured yellow injection.
At the start of 2025, the world was on track to end the Aids pandemic by 2030. However, this progress was disrupted by unprecedented aid cuts from the US, the UK, and other European nations, causing the largest-ever disruptions to HIV responses, from testing to treatment and prevention.
If these aid reductions continue, modelling by The Independent suggests there could be millions more deaths and infections, alongside a doubling of medication-resistant strains. This makes the timing of the Lenacapavir rollout critically important.
Global Deployment and Challenges
Developed by California-based biopharmaceutical company Gilead Sciences, the UN asserts that if properly deployed, this treatment could help reduce new infections to zero and bring about the epidemic's end.
The current plan, funded by the Global Fund to Fight Aids, TB and Malaria, along with the US government and other partners, aims to deliver Lenacapavir to two million people by 2028. While the drug can cost up to $24,000 annually in wealthy nations, it is being provided at a significantly reduced cost to some of the poorest, most at-risk countries.
Historically, life-sustaining antiretroviral therapy was available in the West for a full decade before reaching sub-Saharan Africa, resulting in countless lost lives and contributing to the current crisis. "This has been a defining moment for the Aids epidemic," says Dianne Stewart from the Global Fund. "We have been fighting for equitable access to new tools since the beginning, and this is the first time in history that we have got it right."
Eswatini's Progress and Setbacks
Eswatini, formerly known as Swaziland, is the first country to receive these injections. It has made substantial efforts, reducing new HIV infections from a peak of 21,000 annually two decades ago to 4,000 in 2023, according to UN data. Nevertheless, approximately a quarter of Swazis aged 15 to 49 are living with HIV, based on the latest figures from the US Centers for Disease Control.
David Maseko of HealthPlus for men, a charity supporting key populations such as LGBT+ communities, explains that aid cuts led to the closure of all 15 mobile charity clinics used by Lianne and others. This has resulted in a surge of individuals, including high-risk groups, going without HIV medication and PrEP—a trend occurring across Sub-Saharan Africa.
"There are a lot of gaps now. We are even struggling to do community testing," he notes. For him, a twice-yearly injection that could help curb the recent infection increase is "simply a game changer."
Arianna, a 17-year-old forced into sex work after her mother's death and leaving an abusive home, concurs. "This is lifesaving for us," she states while receiving the injection. She describes the near-impossibility of obtaining daily PrEP pills from public facilities due to prejudice against sex workers and limited earnings for transport. "That is why today I decided to come here. To me, this is the best way to help myself, to survive."
Concerns Over Limited Reach
Despite these advances, worries remain that without adequate global investment to protect a critical mass of people, the impact will be constrained. Currently, delivery targets only nine countries, though expansion plans exist. Lenacapavir has not yet been licensed or procured for large parts of Latin America, where infection rates are climbing.
"We have seen in the past that piecemeal solutions, especially for infectious diseases, do not work," adds Stewart from the Global Fund. "As we saw during Covid, you cannot solve it in one country and think it is done while others do not have access."
At a Medecins Sans Frontieres (MSF) clinic outside the capital, country lead Dr Diojki Bahati reports they were allocated only 50 doses and have had to turn patients away. He emphasises that even reaching two million people over the next three years is "far below the global need."
UNAIDS indicates that to tackle the pandemic, 20 million people need to be on PrEP in the coming years. "Two million people over three years is less than 10 per cent of that target," Dr Bahati notes.
He further explains that there are no alternative procurement systems for organisations like MSF, which have been denied direct purchasing rights. While generic manufacturing licences have been granted to about six manufacturers to supply 120 countries and territories in the upcoming year, this excludes numerous low- and middle-income nations, such as Brazil, Peru, and Mexico, where up to 20% of new infections occur.
Financial Implications and Future Hopes
Dr Bahati stresses that proper funding and government support are essential for the rollout, even amid aid cuts, as it will be more cost-effective long-term. In 2024, there were at least 1.3 million new HIV infections. Carmen Pérez Casas from health initiative Unitaid calculates that these additional infections could incur an extra $52 million annually if everyone receives antiretroviral treatment, leading to lifetime costs of approximately $2 billion. As transmission rises, these expenses will accumulate exponentially.
"This is a fraction of what it could cost to deliver Lenacapavir... at the scale required to bend the curve of the epidemic," she adds.
Back at the Eswatini clinic, demand is evident. Lianne and Arianna breathe sighs of relief post-injection, reassured of their protection for now. "We beg that they do not get tired of helping us," Lianne pleads as her appointment concludes. "If they are cutting the funding, it means we will be exposed and die of HIV. Please help."









