HIV Vaccine Trial Rescued After Trump's Aid Cuts, Yet Delays Linger
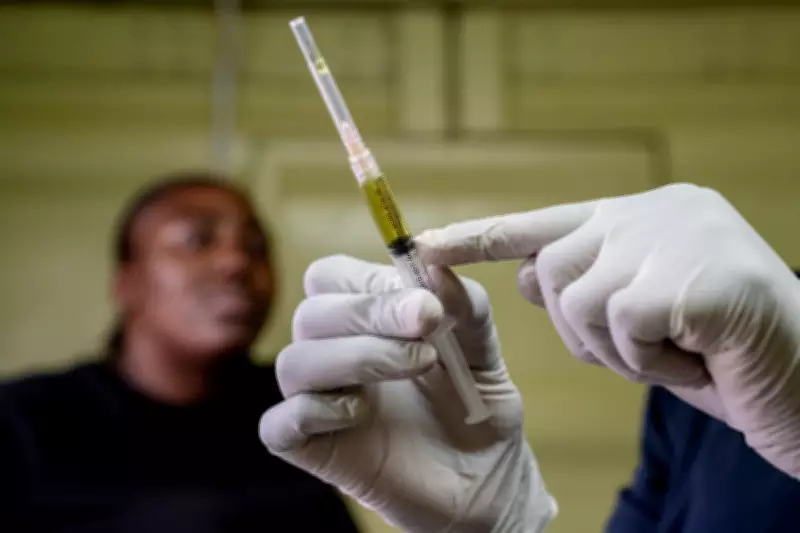
In a clinic in Cape Town earlier this year, a woman rolled up her sleeve, marking the first enrollment in a pivotal HIV treatment trial on African soil. This moment, however, almost never happened. Researchers had spent months in uncertainty after the programme, known as BRILLIANT 011, faced a sudden stop-work order from Washington.
The trial, part of an Africa-led consortium aiming to develop a potential HIV vaccine, was days from its original launch when funding was slashed. As part of Donald Trump's efforts to reduce US aid upon his return to the White House, a $45 million grant from the United States Agency for International Development (USAID) was cancelled abruptly, halting the project overnight.
Rebuilding Against the Odds
Thanks to a swift response involving South African government funding, backing from the Gates Foundation, and support from the Wellcome Trust—totalling around $33 million—the BRILLIANT Consortium managed to rebuild. The trial is now operational, but the interruption has come at a significant cost.
Penny Moore, a virologist at the University of the Witwatersrand in Johannesburg, highlights the knock-on effects. Her lab, equipped with American-funded tools bearing "From the American People" stickers, now faces slowed progress due to disrupted collaborations with scientists in the US and Europe. "Getting reagents from those labs and dealing with reduced engagement has really slowed us down," Moore explains. "The training network that elevated a generation of African scientists came to an abrupt halt."
She notes that while she avoided layoffs, she is "in the minority," and the stoppage compounded logistical challenges. "Trials are so difficult to set up," Moore says. "Starting and stopping costs far more than you'd think, as each new trial requires regulatory approval. This has cost my consortium a whole year."
The Human Toll of Funding Gaps
This tension between scientific momentum and systemic fragility echoes across the global HIV landscape. In Uganda, a mother living with HIV, who wishes to remain anonymous, describes a personal collapse. "After the aid cuts, I went a long time without my antiretrovirals," she shares. "It was risking my life and my child's life. We now lack follow-up care and struggle to find resources."
The distance between breakthroughs and impact is stark—measured not in dollars, but in a mother rationing medication in Kabale while researchers in Johannesburg push forward with a vaccine that could one day eliminate such worries.
Innovations in Prevention and Delivery
The BRILLIANT 011 vaccine aims to train the immune system to recognise HIV through broadly neutralising antibodies, targeting diverse global strains. Moore describes the virus as making "every mistake it can, every single day," necessitating a sequential vaccine approach that nudges the immune system down an unnatural path.
"We have vaccinated the first seven," Moore continues. "It will take time for data, and with a sequential vaccine, we must wait for preclinical results to design boosters. Every element is slower than I wish it were, always for good reasons, but progress can be slow."
Africa remains the epicentre of HIV, with viral strains often absent from global research. Moore emphasises the equity gap: "South African populations are completely uncharacterised. Genetic diversity here is huge and missing from databases, highlighting the need for vaccines that work where they're needed most."
Lenacapavir: A Transformative Tool with Challenges
Simultaneously, another breakthrough is unfolding in southern Africa: lenacapavir, a twice-yearly preventative jab offering near-total protection from HIV. Described as the nearest thing to a vaccine, it could change the epidemic's course, but delivery systems are under strain.
In Zimbabwe, young women queued in heat for the jab, among the first in a public health programme. Professor Quarraisha Abdool Karim, who helped develop PrEP, notes that in sub-Saharan Africa, women and girls account for 63% of new infections, often during adolescence. "It's a period of experimentation and passion," she says. "Lenacapavir fits into real life, unlike daily pills that can be too demanding."
A recent deal promises lenacapavir at $40 per person per year in 120 low- and middle-income countries, a price reduction of over 99%. However, gaps remain. Antonio Flores of Médecins Sans Frontières points out that regions like Eastern Europe and Latin America are excluded from licensing agreements, affecting 20% of new infections.
Carolyn Amole of the Clinton Health Access Initiative calls lenacapavir a watershed moment. "It's the most significant breakthrough in HIV prevention history," she says, adding that political readiness exists in places like Zambia and Kenya. Yet, she warns that without coordinated investment in rollout, "even the most transformative tool will sit on the shelf."
Looking Ahead with Cautious Optimism
Ismail Harerimana, a community health worker in Uganda who lost his job due to USAID cuts, describes the human cost: clinics left unattended, wrong medicines dispensed, and lives lost. "We have lost so many children," he laments.
Rachel Bonnifield of the Centre for Global Development worries about prevention for politically sensitive populations, such as sex workers and gay men, where governments may be less eager to serve.
Despite these challenges, Moore remains optimistic. "The field of HIV/AIDS research has made more progress in the last five years than for a while," she reflects. "But we still acknowledge there is a long way to go." The battle to end the AIDS pandemic continues, hinging on sustained funding, equitable access, and resilient systems.









