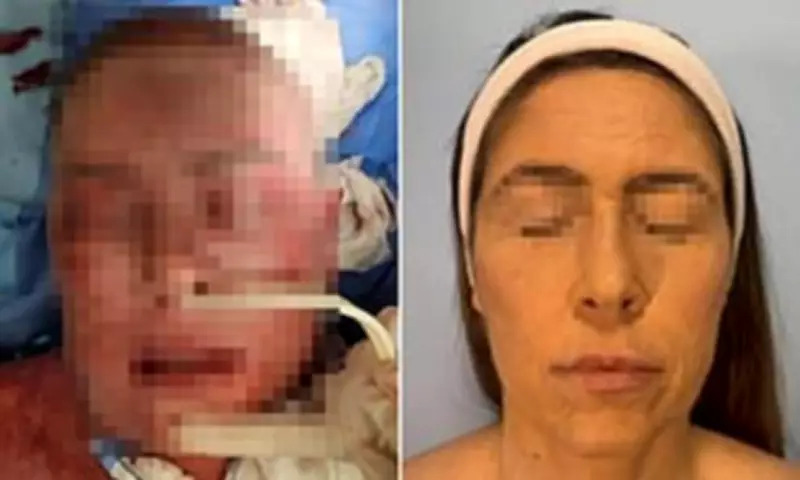
A 42-year-old woman was left with severe burn-like marks, extensive blisters, and significant scarring across her face for more than two months following a rare and life-threatening reaction to a commonly prescribed mood stabiliser. Medical professionals confirmed that the patient, who chose to remain anonymous, developed this dangerous condition after taking lamotrigine, a drug frequently used to treat bipolar disorder and epilepsy.
Widespread Use and Severe Reaction
Lamotrigine is a medication with millions of prescriptions issued annually in the United Kingdom, and it is estimated that around two million individuals in the United States rely on it for treatment. In this case, the woman's medical team believes the drug triggered toxic epidermal necrolysis (TEN), an extremely severe skin reaction that rapidly spread across her face, head, neck, and torso.
Toxic epidermal necrolysis is most often associated with medications such as anti-epileptic drugs, antibiotics, and anti-inflammatories. Although it is exceptionally rare, this condition can be fatal, highlighting the critical nature of such adverse reactions.
Progression of Symptoms and Hospitalisation
The woman had been prescribed lamotrigine to manage depression, and she first began experiencing symptoms approximately three weeks after starting the medication. These symptoms progressively worsened over time, leading to a severe deterioration in her condition.
She was eventually rushed to intensive care at Hospital Beneficencia Portuguesa in São Paulo, Brazil. By the time of her admission, her face was almost entirely covered in painful lesions, causing significant distress and discomfort.
Shocking Visual Documentation
Images captured during her hospital stay reveal the alarming progression of the condition. On the first day of admission, her face was covered in raw, painful lesions. By the second day, her skin had turned a dark purple hue and had begun to peel extensively across her facial area.
By day four, the skin had blackened, with burn-like damage most severe around her mouth. In the initial days of treatment, her condition appeared to deteriorate further as layers of skin continued to break down, complicating her recovery process.
Treatment and Recovery Journey
Doctors treated her with multiple antibiotics and applied an antibacterial biomaterial to support tissue regeneration and promote healing. After four days, she began to show signs of improvement, and her care continued with regular monitoring to ensure stability.
Following one month of treatment, the woman's face showed signs of improvement, though it remained heavily scarred. She remained in hospital for a total of 66 days, with her skin gradually healing over this extended period.
At a follow-up appointment six months after discharge, doctors described the recovery of the affected areas as 'excellent', indicating a positive outcome despite the severity of the initial reaction.
Previous Cases and Awareness
While such reactions to lamotrigine are rare, they have been reported in the past. Earlier this year, the Daily Mail highlighted the case of Emily McAllister, a mother from Chicago who lost approximately 90 per cent of her skin, including on her face, after developing a similar condition known as Stevens-Johnson syndrome, which is also linked to the drug.
Ms McAllister was left permanently blind despite undergoing multiple reconstructive surgeries. She first noticed symptoms around 16 days after starting the medication, including red, dry eyes and swelling of her lips and face, which quickly escalated into a painful, spreading rash.
She recounted, 'I thought I wasn't sure what it was, I just knew something didn't feel right. The second day, my sister came to my house, and I was pretty incoherent. I was having a hard time breathing and was disoriented. That's when the rash started to spread across my face and left me with blisters. It was very painful.'
As her condition worsened, she was admitted to hospital and placed in a burns unit for seven weeks. Over the next three years, she endured the loss of 87 per cent of her skin and underwent a series of major procedures, including eyelid reconstruction, a stem cell transplant, a salivary gland transplant, and multiple surgeries to treat internal scarring.
She added, 'There's not enough awareness about SJS – you trust your doctor, then something like this happens. Before this, I never would've worried about any medication prescribed by a doctor.'









